Anniversary
Storybook Entertainment, the full-time entertainment company that has brought joy to more than 3,000 birthday parties and numerous public events, is celebrating its 10-year anniversary on Saturday, …
ON TOUR
Megadeth is bringing its live show to North America with a nationwide fall tour, Destroy All Enemies, which will include a Phoenix stop.
GRAND JURY
Two teens have been indicted in what the Maricopa County Attorney’s Office called an “ambush” shooting of a Phoenix police officer.
Mathew Rodriguez, 17, has been charged as an …
Valley & State
An Arizona judge has declared a mistrial in the case of rancher accused of fatally shooting a Mexican man on his property near the U.S.-Mexico border. Jurors could not reach consensus on last …
courts
Two First Amendment advocacy groups are asking a federal district court to throw out a case that a Peoria Unified School District governing board member filed against her own school board.
Election 2024
PHOENIX — Progress Arizona is launching a campaign to deny new terms to two of the state Supreme Court justices who voted earlier this month to allow the 1864 law on abortion to once again be …
2024 ELECTION
As a result of a legal challenge to his nominating petition signatures last week, Jamie Aldama dropped out of the Glendale mayoral race Monday afternoon, just before a court hearing.
…
ON TOUR
Acclaimed Mexican singer-songwriter Eden Muñoz will bring his Como en los Viejos Tiempos tour to Phoenix.
artifact
A rare piece of automotive military history has been retrieved and revitalized in north Peoria, and now it will be preserved in a California museum for future generations to enjoy.
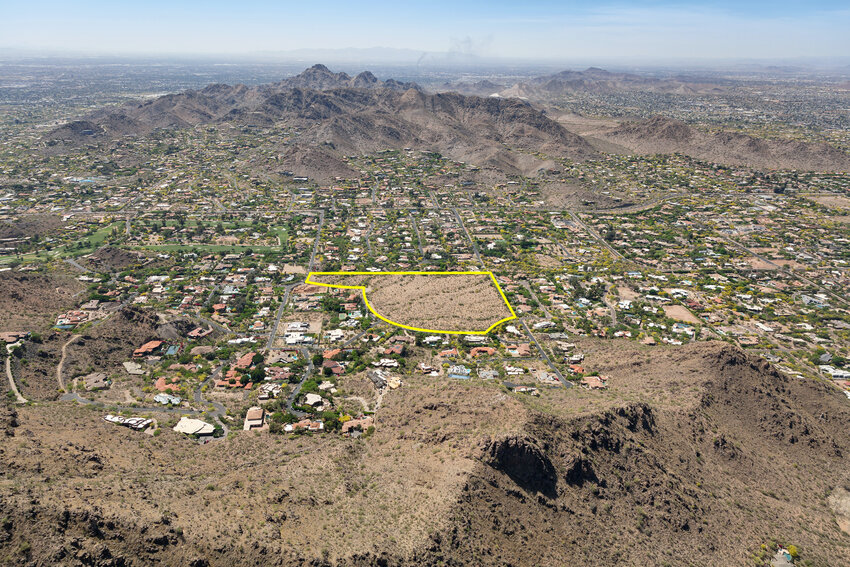
real estate
The 27-acre undeveloped parcel of land near Mummy Mountain in the Town of Paradise Valley was sold last week for a record-breaking $42 million — and it could have sold higher.
For nearly …
education
??In keeping with its attempts to keep students using some of the latest technology hardware, the Chandler Unified School District has another large purchase planned for discussion and action this …
NEIGHBORS
Sonar Technician (Surface) 2nd Class Kevin Perez, from Phoenix, blows a signal whistle aboard the Arleigh Burke-class guided-missile destroyer USS Dewey.
Read more







!role~Preview!mt~photo!fmt~JPEG%20Baseline)













!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
















!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)
!role~Preview!mt~photo!fmt~JPEG%20Baseline)